Professionally Reviewed by Dt Chen Zi Xin, Registered Dietitian
You have probably come across the words probiotics and prebiotics on supplement labels or yogurt containers, or perhaps even short-chain fatty acids (SCFAs) in newer discussions about gut health.
They are all connected, but each plays a unique role in supporting a healthy digestive system.
Understanding how they differ, and how they work together, helps explain why gut health isn’t just about taking one or few types of supplements, but about using them nurture the entire gut ecosystem in the body.
The Gut Microbiome: The Starting Point
Inside your digestive tract lives a vast community of microorganisms called the gut microbiome. It is an ecosystem that contains trillions of bacteria, fungi, and other microbes that interact with the food you eat and with your body’s systems (1, 2).
When this ecosystem is balanced, it supports digestion, nutrient absorption, immune defense, and even mental health (3, 4). When it’s disrupted due to poor diet, antibiotics, stress, or illness, it can lead to bloating, irregular bowel habits, inflammation, and other health issues (3).
To keep this complex system in balance, three main factors come into play: probiotics, prebiotics, and short-chain fatty acids (SCFAs).
Probiotics: The “Good” Gut Bacteria
Probiotics are live beneficial bacteria (also known as good gut bacteria) that help maintain a healthy microbial environment in the gut. Think of them as friendly reinforcements that strengthen your gut’s natural defence (5, 6).
Common Probiotic Sources (5)
- Fermented foods: Yogurt, kefir, kimchi, miso, sauerkraut, and tempeh.
- Dietary supplements: Strains such as Lactobacillus, Bifidobacterium
What They Do (5, 6, 7, 8)
- Restore microbial balance: After antibiotics or illness, probiotics help replenish good gut bacteria that was destroyed by antibiotics or inflammation.
- Support digestion: Certain strains aid in breaking down lactose, fiber, and other nutrients.
- Enhance immunity: They interact with immune cells in the intestinal wall to regulate inflammation.
Probiotics are living organisms, so their benefits depend on strain type, survival through stomach acid, and their ability to colonise the gut.
Prebiotics: The “Food” to Feed Good Gut Bacteria
Prebiotics are non-digestible dietary fibers that act as food for probiotics. They are not living organisms, but substances that nourishes the growth and activity of beneficial microbes (9).
Common Prebiotic Sources (9, 10)
1. Natural foods: Garlic, onions, leeks, asparagus, bananas, apples, and barley.
2. SCFA-friendly fibers: Inulin, fructooligosaccharides (FOS), resistant starch, pectin, and guar gum.
What They Do (9, 11, 12, 13)
- Feed good bacteria: Prebiotics fuel the beneficial strains already in your gut.
- Boost SCFA production: When gut bacteria ferment prebiotics, they produce short-chain fatty acids like butyrate, acetate, and propionate.
- Improve gut barrier strength: Prebiotics indirectly support a stronger intestinal lining and more stable gut environment.
Essentially, probiotics need prebiotics to thrive — and together, they lay the foundation for a balanced, resilient gut microbiome (9, 11).
Short-Chain Fatty Acids: The Beneficial “Outcome” Produced by Probiotics and Prebiotics
Here’s where short-chain fatty acids (SCFAs) enter the picture. SCFAs — mainly acetate, propionate, and butyrate — are metabolites, or byproducts, formed when the good gut bacteria (probiotics) ferment prebiotics in the colon.
These SCFAs are what our gut strives to create through a balanced microbiome and sufficient fiber intake, because they play various important functions for the gut and body, such as (12, 14, 15, 16),
- Fuel for gut cells: SCFA like Butyrate provides up to 70% of the energy used by colon cells, helping them grow and repair.
- Anti-inflammatory support: SCFAs help regulate immune responses and reduce inflammation in the intestinal wall.
- Gut Barrier protection: They strengthen the tight junctions that keep the gut lining intact, preventing “leaky gut.”
- Improve bowel motility and movement: They help regulate bowel movements to improve symptoms such as bloating, constipation and diarrhea.
- Metabolic and brain effects: SCFAs influence appetite, glucose regulation, and even communication between the gut and brain through the vagus nerve.
Among these SCFAs, Butyrate is particularly important for colon health as it is the primary energy source for colon cells and plays a critical role in maintaining intestinal health, reducing inflammation, and supporting gut barrier integrity (12, 18, 19). Learn more about Butyrate here:
In essence, probiotics are the workers, prebiotics are their fuel, and SCFAs are the beneficial end products they create—delivering many of the vital outcomes that keep our digestive and immune systems functioning at their best.
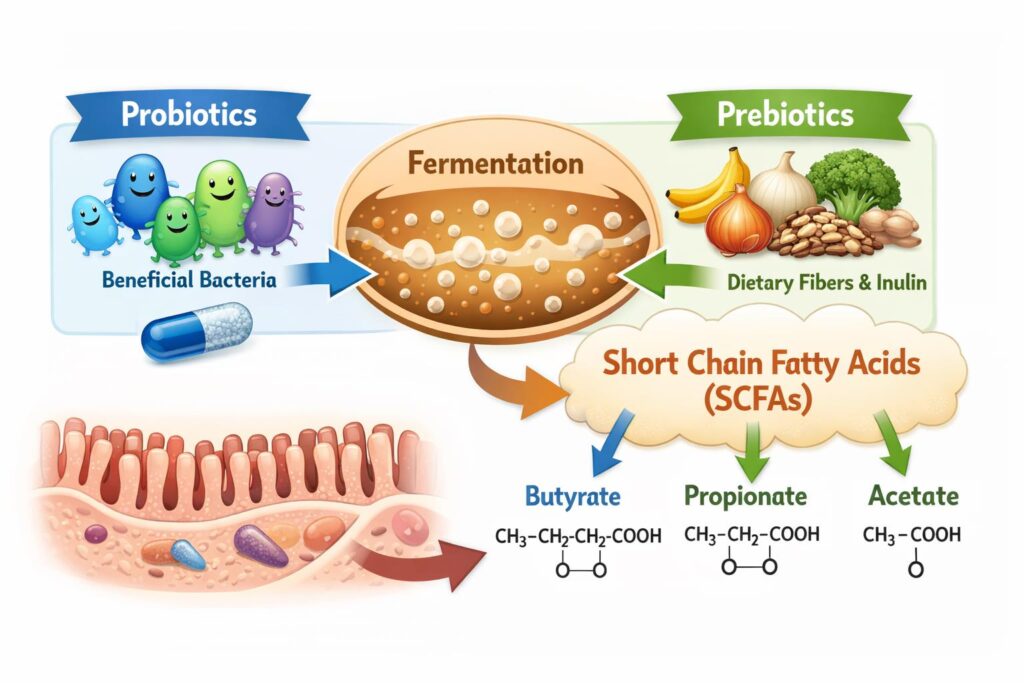
How They Work Together
Here’s how the synergy unfolds:
- Prebiotics (fiber) enter the colon undigested.
- Probiotics (bacteria) ferment those fibers.
- This fermentation process produces SCFAs such as butyrate.
- SCFAs then nourish colon cells, reduce inflammation, and maintain gut balance.
Both elements — prebiotics and probiotics — are therefore essential to complete the cycle that generates SCFAs and sustains intestinal health.
In short, probiotics and prebiotics create the conditions, while SCFAs deliver the benefits — completing the cycle of a healthy, well-functioning gut ecosystem.
When Things Go Out of Balance
When fiber intake is low, or when gut microbiome is disrupted — due to stress, illness, aging, or medication — SCFA production will be affected (20). This can result in:
- Weakened gut barrier and “leaky gut” symptoms
- Increased inflammation and intestinal sensitivity
- Irregular bowel habits or digestive discomfort
Without sufficient dietary fiber, gut bacteria lack the fuel needed to produce short-chain fatty acids (SCFAs). Conversely, without a healthy gut microbiome, even a high-fiber diet cannot be efficiently utilised. Over time, this imbalance affects not only digestion, but also metabolism and immune regulation (20).
Many of us today may not produce enough SCFAs, often due to inadequate fiber intake, poor dietary habits, or disruptions in gut bacteria caused by lifestyle factors, sickness and digestive disorders such as Irritable Bowel Syndrome (IBS) or Inflammatory Bowel Disease (IBD) (12, 17).
How to Support the Cycle Naturally
You can support this gut ecosystem by nurturing every part of the chain:
- Eat more fiber: Aim for at least 25–30 grams per day from a variety of fiber sources. This is supported by the Institute of Medicine, the Academy of Nutrition and Dietetics, and major U.S. guidelines (21).
- Include fermented foods: Add yogurt, kefir, kimchi, or sauerkraut to your diet to introduce beneficial bacteria.
- Consider Butyrate supplements: Due to lifestyle, digestive disorders or certain health conditions such as chronic illness or antibiotic use, where SCFAs may be difficult to produce, Butyrate supplements can be used to restore gut balance.
Conclusion
Probiotics, prebiotics, and short-chain fatty acids are all required of the digestive ecosystem. Probiotics are the beneficial bacteria, prebiotics the fibers that feed them, and SCFAs the health results of synergy between Probiotics and Prebiotics.
By eating a fiber-rich, balanced diet and maintaining a diverse microbiome, you enable this natural cycle to thrive — supporting gut comfort, nutrient absorption, immune strength, and overall wellbeing from the inside out.
About the Reviewer
Chen Zi Xin is a registered dietitian of the Malaysian Dietitians’ Association (MDA) and a member of the Malaysian Allied Health Professional Council (MAHPC). With rich experience in nutraceuticals and healthcare marketing, she contributes to product development and professional nutrition training, including hospital nurse and pharmacist training programs. She is driven by the belief that informed nutrition transforms daily health outcomes.
References :
- Gilbert, J. A., Blaser, M. J., Caporaso, J. G., Jansson, J. K., Lynch, S. V., & Knight, R. (2018). Current understanding of the human microbiome. Nature medicine, 24(4), 392–400. https://doi.org/10.1038/nm.4517
- Cleveland Clinic. (n.d.). Gut microbiome. Retrieved October 2025, from https://my.clevelandclinic.org/health/body/25201-gut-microbiome
- Conlon, M. A., & Bird, A. R. (2014). The impact of diet and lifestyle on gut microbiota and human health. Nutrients, 7(1), 17–44. https://doi.org/10.3390/nu7010017
- Cryan, J. F., & Dinan, T. G. (2012). Mind-altering microorganisms: The impact of the gut microbiota on brain and behaviour. Nature Reviews Neuroscience, 13(10), 701–712. https://doi.org/10.1038/nrn3346
- Cleveland Clinic. (n.d.). Probiotics: What they are, types & benefits. Retrieved October 2025, from https://my.clevelandclinic.org/health/articles/14598-probiotics
- Hill, C., Guarner, F., Reid, G., Gibson, G. R., Merenstein, D. J., Pot, B., Morelli, L., Canani, R. B., Flint, H. J., Salminen, S., Calder, P. C., & Sanders, M. E. (2014). The International Scientific Association for Probiotics and Prebiotics consensus statement on the scope and appropriate use of the term probiotic. Nature Reviews Gastroenterology & Hepatology, 11(8), 506–514. https://doi.org/10.1038/nrgastro.2014.66
- Ouwehand, A. C., DongLian, C., Weijian, X., Stewart, M., & Stewart, T. (2016). Probiotic and other functional microorganisms: Types, uses, and health benefits. Microbial Ecology in Health & Disease, 27(1), 30259. https://doi.org/10.3402/mehd.v27.30259
- Sanders, M. E., Merenstein, D. J., Merrifield, C. A., Hutkins, R., & Reid, G. (2018). Probiotics for human use: The current evidence. Gut Microbes, 9(4), 347–364. https://doi.org/10.1080/19490976.2018.1462425
- Cleveland Clinic. (2022) What Are Prebiotics and What Do They Do? Retrieved October 2025, from https://health.clevelandclinic.org/what-are-prebiotics
- Slavin, J. (2013). Fiber and prebiotics: Mechanisms and health benefits. Nutrients, 5(4), 1417–1435. https://doi.org/10.3390/nu5041417
- Gibson, G. R., Hutkins, R., Sanders, M. E., Prescott, S. L., Reimer, R. A., Salminen, S. J., Scott, K., Stanton, C., Swanson, K. S., Cani, P. D., Verbeke, K., & Reid, G. (2017). Expert consensus document: The International Scientific Association for Probiotics and Prebiotics (ISAPP) consensus statement on the definition and scope of prebiotics. Nature Reviews Gastroenterology & Hepatology, 14(8), 491–502. https://doi.org/10.1038/nrgastro.2017.75
- Canani, R. B., Costanzo, M. D., Leone, L., Pedata, M., Meli, R., & Calignano, A. (2011). Potential beneficial effects of butyrate in intestinal and extraintestinal diseases. World Journal of Gastroenterology, 17(12), 1519–1528. https://doi.org/10.3748/wjg.v17.i12.1519
- Cummings, J. H., & Macfarlane, G. T. (2002). Gastrointestinal effects of prebiotics. British Journal of Nutrition, 87(S2), S145–S151. https://doi.org/10.1079/BJN2002530
- Liu, H., Wang, J., He, T., Becker, S., Zhang, G., Li, D., & Ma, X. (2018). Butyrate: A Double-Edged Sword for Health?. Advances in nutrition (Bethesda, Md.), 9(1), 21–29. https://doi.org/10.1093/advances/nmx009
- Mishra, S. P., Jain, S., Wang, B., Wang, S., Miller, B. C., Lee, J. Y., Borlongan, C. V., Jiang, L., Pollak, J., Taraphder, S., Layden, B. T., Rane, S. G., & Yadav, H. (2024). Abnormalities in microbiota/butyrate/FFAR3 signaling in aging gut impair brain function. JCI insight, 9(3), e168443. https://doi.org/10.1172/jci.insight.168443
- Dalile, B., Van Oudenhove, L., Vervliet, B., & Verbeke, K. (2019). The role of short-chain fatty acids in microbiota–gut–brain communication. Nature Reviews Gastroenterology & Hepatology, 16(8), 461–478. https://doi.org/10.1038/s41575-019-0157-3
- den Besten, G., van Eunen, K., Groen, A. K., Venema, K., Reijngoud, D. J., & Bakker, B. M. (2013). The role of short-chain fatty acids in the interplay between diet, gut microbiota, and host energy metabolism. Journal of Lipid Research, 54(9), 2325–2340. https://doi.org/10.1194/jlr.R036012
- Liu, H., Wang, J., He, T., Becker, S., Zhang, G., Li, D., & Ma, X. (2018). Butyrate: A Double-Edged Sword for Health?. Advances in nutrition (Bethesda, Md.), 9(1), 21–29. https://doi.org/10.1093/advances/nmx009
- Peng, L., Li, Z. R., Green, R. S., Holzman, I. R., & Lin, J. (2009). Butyrate enhances the intestinal barrier by facilitating tight-junction assembly via activation of AMP-activated protein kinase. The Journal of Nutrition, 139(9), 1619–1625. https://doi.org/10.3945/jn.109.104638
- Fu, J et al. (2022). Dietary Fiber Intake and Gut Microbiota in Human Health. Microorganisms, 10(12), 2507. https://doi.org/10.3390/microorganisms10122507
- Daley, S. F., & Shreenath, A. P. (2025). The Role of Dietary Fiber in Health Promotion and Disease Prevention: A Practical Guide for Clinicians. In StatPearls. StatPearls Publishing.