Reviewed by Dt Chen Zi Xin, Registered Dietitian
Butyrate is a short-chain fatty acid (SCFA) naturally produced when the good gut bacteria ferment dietary fiber in the colon (1). It serves as the main energy source for colon cells, helps maintain the gut (intestinal) barrier, and has anti-inflammatory properties (2).
In order to produce SCFAs, one must have a good gut microbiota with sufficient good gut bacteria and dietary fiber intake via a well, balanced diet (1, 3, 4).
However, many of us today may not produce enough butyrate — often due to poor fiber intake, or disrupted gut microbiota due to poor diet, lifestyle, or digestive disorders such as Irritable Bowel Syndrome (IBS) and Inflammatory Bowel Disease (IBD) (14,15).
This article explores the types of butyrate supplements available, how they work, and what to consider when choosing one.
Why Take Butyrate Supplements?
When your gut is healthy and your diet is rich in dietary fiber, the colon naturally produces enough butyrate to sustain the colon health (1, 3, 4).
But when the gut microbiome is disrupted or inflamed, or fiber intake is inadequate, butyrate levels may drop — leading to inflammation, discomfort, and weakened gut barrier function (2).
Butyrate supplements can therefore be used as a quick, rich source of this essential SCFA, in order to restore balance and support intestinal health, even when our gut or diet is not fit to produce them.
Some benefits of using Butyrate supplements (5, 6, 7, 8, 9),
- Support colon lining repair and barrier strength
- Reduce inflammation in the colon.
- Normalize bowel movements and relieve irregularity.
- Improve overall digestive comfort and microbial balance.
While it is always best for all nutrients — including short-chain fatty acids (SCFAs) — to be obtained through a balanced diet and whole food sources, supplementation can be an useful option for individuals with persistent gut issues (such as IBS, IBD, Leaky Gut), poor diet and lifestyle, or those recovering from antibiotic use (14,15).
Main Types of Butyrate Supplements
Butyrate supplements come in several forms that differ in absorption, release profile, and tolerability, such as sodium butyrate, calcium butyrate or calcium-magnesium butyrate.
Each delivers the same core molecule — butyric acid — but is bound to different minerals or formulated using specific delivery technologies that determine how effectively it reaches the colon.
Sodium Butyrate
Sodium butyrate is one of the earliest and most widely studied forms of butyrate supplementation (5). It combines butyric acid with sodium.
While effective and well-researched, this form contains a significant amount of sodium, which may not be suitable for individuals with hypertension, kidney conditions, or those already consuming diets high in sodium, which is a common concern in modern populations.
Calcium Butyrate or Calcium-Magnesium Butyrate
Calcium butyrate and Calcium–Magnesium butyrate are mineral-bound forms in which butyric acid is combined with either calcium alone, or with both calcium and magnesium. These sodium-free alternatives could be healthier options for individuals who need to limit sodium intake.
For Calcium-Magnesium Butyrate, the addition of magnesium may occasionally cause loose stools or mild cramping if taken in excess, as magnesium naturally has a mild laxative effect (13).
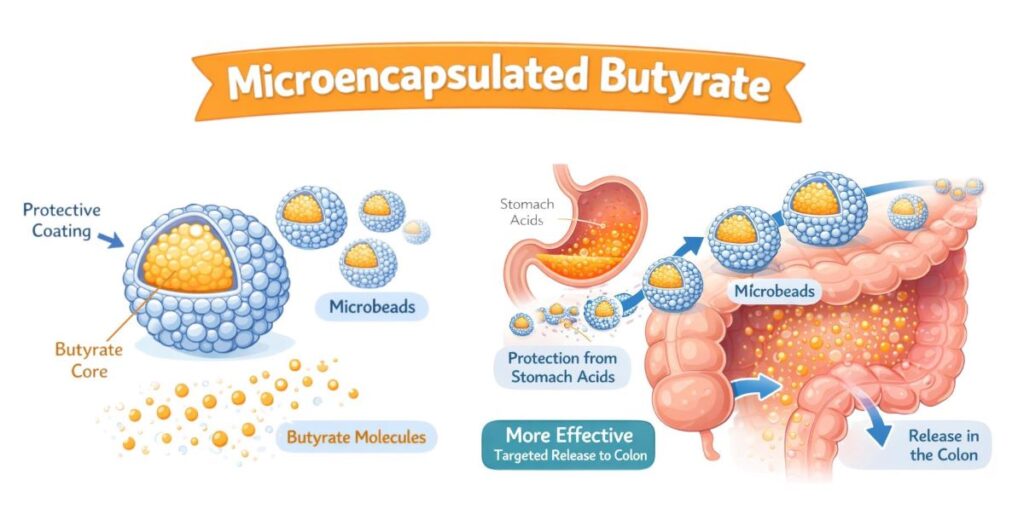
Go for Microencapsulated Butyrate for Better Outcomes
Microencapsulation represents a major advancement in butyrate supplement technology. By coating butyrate molecules with a lipid or polymer layer, this process shields them from stomach acid and allows more of the compound to reach the colon intact, where it provides the greatest benefit (11, 12).
Clinical studies have demonstrated that microencapsulated sodium butyrate can significantly reduce symptoms in individuals such as those with irritable bowel syndrome, as compared with conventional butyrate salts (10).
This targeted delivery not only enhances absorption and bioavailability but also improves consumption compliance by masking butyrate’s naturally strong odor and taste (10). The gradual release achieved through microencapsulation supports longer intestinal action, better gut barrier integrity and more sustainable digestive comfort (10, 11).
What to Look for When Choosing a Butyrate Supplement
- Formulation: Look for microencapsulated forms to ensure more targeted delivery to the colon before it gets destroyed by stomach acid.
- Mineral Type: Consider calcium or magnesium butyrate if you wish to limit sodium intake.
- Dosage and Tolerance: Start with a lower dose and increase gradually, as high doses may cause bloating for some, especially those with digestive disorders.
- Professional Guidance: Always consult a healthcare provider before starting supplementation, particularly if you have underlying health conditions or are taking medications.
Conclusion
Butyrate supplements provide a practical way to support colon health, especially when natural SCFA production is low due to various factors. While sodium, calcium, and magnesium butyrate all supply the same active molecule, their differences in mineral content, absorption, and release mechanisms influence how well they work.
Among the available options, calcium butyrate in a microencapsulated form stands out as a well-balanced, sodium-free choice with improved stability and targeted delivery. When paired with a fiber-rich diet that naturally encourages SCFA production, butyrate supplementation can help restore digestive comfort and strengthen gut integrity from within.
About the Reviewer
Chen Zi Xin is a registered dietitian of the Malaysian Dietitians’ Association (MDA) and a member of the Malaysian Allied Health Professional Council (MAHPC). With rich experience in nutraceuticals and healthcare marketing, she contributes to product development and professional nutrition training, including hospital nurse and pharmacist training programs. She is driven by the belief that informed nutrition transforms daily health outcomes.
References :
- Healthline Editorial Team. (2025, August 26). The proven and potential benefits of butyric acid. Healthline. https://www.healthline.com/health/butyric-acid
- Liu, H., Wang, J., He, T., Becker, S., Zhang, G., Li, D., & Ma, X. (2018). Butyrate: A Double-Edged Sword for Health?. Advances in nutrition (Bethesda, Md.), 9(1), 21–29. https://doi.org/10.1093/advances/nmx009
- Mueller, N. T., Zhang, M., Juraschek, S. P., Miller, E. R., & Appel, L. J. (2020). Effects of high-fiber diets enriched with carbohydrate, protein, or unsaturated fat on circulating short chain fatty acids: results from the OmniHeart randomized trial. The American journal of clinical nutrition, 111(3), 545–554. https://doi.org/10.1093/ajcn/nqz322
- Yang, Q., Liang, Q., Balakrishnan, B., Belobrajdic, D. P., Feng, Q. J., & Zhang, W. (2020). Role of Dietary Nutrients in the Modulation of Gut Microbiota: A Narrative Review. Nutrients, 12(2), 381. https://doi.org/10.3390/nu12020381
- Canani, R. B., Costanzo, M. D., Leone, L., Pedata, M., Meli, R., & Calignano, A. (2011). Potential beneficial effects of butyrate in intestinal and extraintestinal diseases. World journal of gastroenterology, 17(12), 1519–1528. https://doi.org/10.3748/wjg.v17.i12.1519
- Chen, J., & Vitetta, L. (2020). Butyrate in inflammatory bowel disease therapy. Correspondence, 158(5), 1511. https://www.gastrojournal.org/action/showPdf?pii=S0016-5085%2820%2930105-0
- Mishra, S. P., Jain, S., Wang, B., Wang, S., Miller, B. C., Lee, J. Y., Borlongan, C. V., Jiang, L., Pollak, J., Taraphder, S., Layden, B. T., Rane, S. G., & Yadav, H. (2024). Abnormalities in microbiota/butyrate/FFAR3 signaling in aging gut impair brain function. JCI insight, 9(3), e168443. https://doi.org/10.1172/jci.insight.168443
- Zhuang, M., Shang, W., Ma, Q., Strappe, P., & Zhou, Z. (2019). Abundance of Probiotics and Butyrate-Production Microbiome Manages Constipation via Short-Chain Fatty Acids Production and Hormones Secretion. Molecular nutrition & food research, 63(23), e1801187. https://doi.org/10.1002/mnfr.201801187
- Cleveland Clinic. (n.d.). Gut microbiome. https://my.clevelandclinic.org/health/body/25201-gut-microbiome
- den Besten, G., van Eunen, K., Groen, A. K., Venema, K., Reijngoud, D. J., & Bakker, B. M. (2013). The role of short-chain fatty acids in the interplay between diet, gut microbiota, and host energy metabolism. Journal of lipid research, 54(9), 2325–2340. https://doi.org/10.1194/jlr.R036012
- Lewandowski, K., Kaniewska, M., Karłowicz, K., Rosołowski, M., & Rydzewska, G. (2022). The effectiveness of microencapsulated sodium butyrate at reducing symptoms in patients with irritable bowel syndrome. Przeglad gastroenterologiczny, 17(1), 28–34. https://doi.org/10.5114/pg.2021.112681
- Tursi, A., Procaccianti, G., De Bastiani, R., Turroni, S., D’Amico, F., Allegretta, L., Antonino, N., Baldi, E., Casamassima, C., Casella, G., Ciuffi, M., De Bastiani, M., Lazzarotto, L., Licci, C., Mancuso, M., Penna, A., Pranzo, G., Sanna, G., Tosetti, C., Zamparella, M., … Picchio, M. (2025). Micro-encapsulated and colonic-release sodium butyrate modulates gut microbiota and improves abdominal pain in patients with symptomatic uncomplicated diverticular disease. Frontiers in medicine, 12,1487892. https://doi.org/10.3389/fmed.2025.1487892
- WebMD (NA). Magnesium – Uses, Side Effects, and More. WebMD. https://www.webmd.com/vitamins/ai/ingredientmono-998/magnesium#dosing
- Conlon, M. A., & Bird, A. R. (2014). The impact of diet and lifestyle on gut microbiota and human health. Nutrients, 7(1), 17–44. https://doi.org/10.3390/nu7010017
- DeGruttola, A. K., Low, D., Mizoguchi, A., & Mizoguchi, E. (2016). Current Understanding of Dysbiosis in Disease in Human and Animal Models. Inflammatory bowel diseases, 22(5), 1137–1150. https://doi.org/10.1097/MIB.0000000000000750






